It is feasible to contextualize Climate Change and Environmental Health content in an existing course and to incorporate relevant assessment questions on this material in order to measure student comprehension of this content, as well as to understand the strengths and opportunities for curricular improvements. This work offers a model for other health professions programs seeking to integrate climate and environmental health into their training.
Introduction: The profound and growing impacts of the climate crisis impinge upon pulmonary health through multiple pathways. Historically marginalized populations are disproportionately exposed to higher levels of air pollution, with social vulnerability amplifying the burden of respiratory illnesses. While most U.S. medical schools cover climate change in their curriculum, strategies for assessing students and evaluating curricula are lacking.
Description of Innovation: Our disseminated climate change and environmental health curriculum includes content integrated into core topics during the Pulmonology course. Students were assessed on their understanding of this content via multiple-choice and essay questions on their final exam. We analyzed these results to evaluate student comprehension of core climate change and environmental health content, including the relationship between environmental exposures and health inequities.
Results: Student performance on the Climate Change and Environmental Health portion of the Pulmonary course final exam exceeded the average performance on the test for both multiple choice and essay questions. One-hundred three (72%) students chose to answer the essay question on climate and health. Students could earn points in six climate and health domains on the essay question. Student essays overwhelmingly demonstrated understanding of the significance of exposure (98%) and epidemiology (96%) in pollution-asthma relationships. Only 4% of students described the effects of air pollution on pulmonary function tests.
Conclusion: These findings highlight successes and opportunities for improvement of the climate change and environmental health curriculum in the Pulmonary course. Results will inform targeted revisions to course content, questions, and scoring rubrics, specifically to enhance understanding of pulmonary function tests in clinical care for patients exposed to air pollution.
Effective incorporation of climate change into medical education is essential to equip future healthcare professionals with the knowledge and skills to recognize, address, and prevent its health impacts. Climate change and air pollution contribute to global morbidity and mortality from respiratory diseases, such as asthma and chronic obstructive pulmonary disease (COPD). Air pollution from human extraction and consumption of fossil fuels, as well as wildfires made more frequent and severe due to climate-driven heat and drought, directly harms lung tissue and worsens lung function. Increased atmospheric carbon dioxide, driven by the burning of fossil fuels, contributes to the amount and strength of pollen produced by some plant species, while climate-driven storms and floods foster mold growth, contributing to allergic respiratory diseases. These environmental exposures directly influence the clinical presentations of common pulmonary diseases (Mireku et al., 2009; D’Amato et al., 2020). Individuals living in communities that have faced discrimination and environmental racism, predominantly communities of color, are exposed to higher levels of ambient air pollution and disproportionate risk of respiratory illness (Smirnova et al., 2023).
As climate change increasingly affects health at both individual and population levels, medical schools are scrambling to train current students for the patient care challenges they will face in practice. A growing body of research demonstrates the rationale and methods for incorporating CCEH content into medical school curricula (Wellbery et al., 2018). Increasingly, US medical schools are teaching climate-related content, with recent data indicating that over 70% of U.S. medical schools include climate change and environmental health (CCEH) topics in their curricula (Blood A, 2024). The initiatives of several U.S. medical schools to incorporate planetary health into preclinical and clinical curricula are collated in the Planetary Health Report Card (PHRC, 2024). Longitudinal approaches aim to equip future physicians with the skills and knowledge to address climate-related health inequities through both clinical practice and advocacy.
Despite this progress in covering CCEH content, student assessment and curricular evaluation strategies are lacking. Past studies evaluating the integration of CCEH into the curriculum have relied on student surveys and qualitative responses outside of the student assessment environment (Hampshire et al., 2021). Although this dimension of evaluation is important to understand student perspectives, the extent to which students absorb and understand CCEH material remains largely unstudied (Trilling, 2024). Determining the uptake and comprehension of CCEH content is crucial for ensuring future healthcare professionals are equipped to address climate-related health challenges effectively.
Emory University was an early adopter of a co-created CCEH curriculum for all medical students. The class of 2024 was the first cohort to receive this integrated and disseminated CCEH content in the required preclinical curriculum in 2020-2021 (Liu et al., 2022). CCEH thread faculty and students worked with the pre-clinical curriculum director, course directors, and faculty across the pre-clinical phase to co-create and integrate CCEH content within existing course work. Much of Emory’s pre-clinical curriculum follows an organ system-based framework. Amongst internal organ systems, lungs are unique in that they interface directly with the external environment or ambient air. Because of the profound implications of climate change and air pollution on pulmonary health and health equity, and the robust evidence-base linking air pollution and climate-driven environmental changes to pulmonary health harms, the Pulmonology course afforded many opportunities to weave CCEH content into existing topics and sessions, both lectures and small groups (Box 1). Students and faculty from the CCEH thread and the Pulmonary course co-created and, in some cases, co-taught these sessions. The Pulmonary course was also among the first courses at Emory University School of Medicine to assess students on CCEH content in the final exam through both multiple-choice and a short-answer essay question.
This study uses first-year medical student performance on the end-of-course pulmonary exam to measure student understanding of the CCEH content and to identify strengths and opportunities for the CCEH curriculum. Additionally, this study examines the feasibility of integrating CCEH content and assessment into an existing course and offers a model for faculty-student collaboration that can be adapted across diverse health professional training programs.
This is a retrospective analysis of a climate change and pulmonary health curriculum for first-year medical students. The evaluation critically considers medical student performance on climate change, air pollution, and pulmonary health topics integrated into the Pulmonology course and final Pulmonary course exam. This study was deemed exempt from review by Emory’s Institutional Review Board based on criterion 45 CFR 46.104(d)(1, 4) (study 00006949).
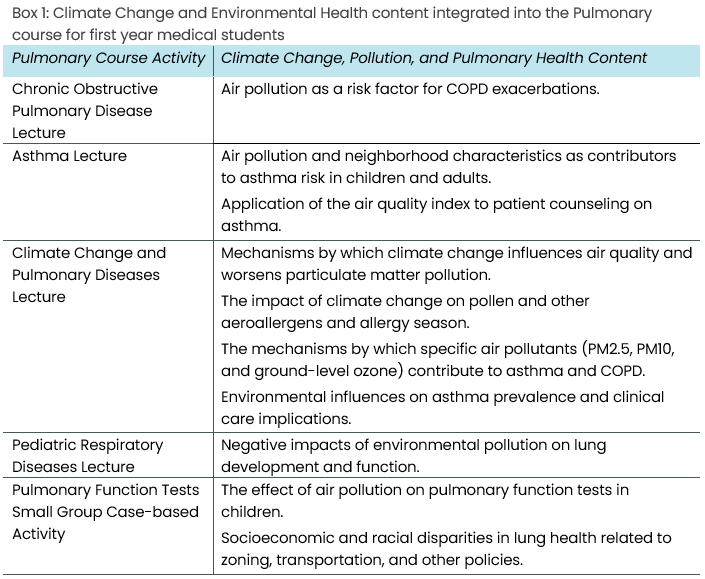
CCEH content was integrated into the Pulmonary course in four pre-existing lectures (“Asthma”, “Chronic Obstructive Pulmonary Disease”, “Pulmonary Pathology”, and “Pediatric Respiratory Disorders”), one free-standing lecture (“Inside Out: Climate Change and Pulmonary Disease”), and one pre-existing small group activity on Pulmonary Function Tests (PFTs). These sessions emphasized the relationship between environmental factors, including climate change, and pulmonary pathology, with an emphasis on pathophysiologic mechanisms and clinical relevance. Topics covered include particulate matter and ozone air pollution, extreme heat, common aeroallergens, and emerging exposures (like algal blooms). The Pulmonary course final exam included multiple-choice questions as well as a short answer component, with the majority of these questions giving students a choice between two essay prompts. The Pulmonary course and CCEH thread leadership co-created and incorporated questions on climate change, air pollution, and pulmonary health into this final exam. Two out of 106 multiple-choice items and one of nine essay questions explicitly assessed learning objectives related to climate change and respiratory health. The course essay exam consisted of nine questions, six of which offered a choice between two unrelated, randomly paired prompts. For one of these pairs, students could choose to answer a question on CCEH or one on pulmonary function testing. The essay on CCEH asked about the intersection of environmental exposures, pulmonary health, and health equity. To answer this question correctly, students needed to apply a framework that includes an individual’s risk of exposure to environmental harms, physiologic factors influencing susceptibility, and ability to adapt to exposures and reduce harm (Smirnova et al., 2023).
The multiple-choice questions were evaluated using routinely collected descriptive measures and a discrimination index, which is a measure of how well the question differentiates between top-performers and low-performers on the test. Performance on the multiple-choice questions was calculated using ExamSoft, the University’s testing platform (ExamSoft, 2025). The Pulmonary Course and CCEH Thread leadership developed a rubric to score the climate change essay question. The rubric reflected six key domains that were emphasized in the course: pathophysiology, epidemiology, and PFTs, as well as exposure, susceptibility, and adaptive capacity (the components of the environmental health vulnerability framework emphasized throughout the CCEH thread as applied to the Pulmonology Course).
Using this rubric, student graders from senior classes (and unaffiliated with the course or thread) scored the essay question, assigning a grade of 0-4. Each essay was graded by a designated student grader, with faculty spot-checking for consistency, minimizing the likelihood of grading errors. Authors did not have access to the application of the rubric in the school’s official grading process. Therefore, to better understand student performance across the core domains as defined in the rubric for this study, two independent student reviewers from senior classes and affiliated with the CCEH thread performed an independent evaluation of de-identified student responses. Student reviewers analyzed which core domains (pathophysiology, epidemiology, PFTs, exposure, susceptibility, and adaptive capacity) the essay responses adequately covered, assigning a score of 0 (not addressed or partially addressed) to 1 (demonstrated understanding). Partial credit was not given. Discrepancies between the two reviewers were resolved by a third reviewer, the CCEH Thread Director. The reviewers analyzed the frequency of student-demonstrated application of content across each domain.
A total of 144 students of the 148 members of the class of 2026 took the Pulmonary course exam before this analysis. Of these students, 104 (70%) identify as female, 44 (30%) identify as male, 29 (20%) are dual-degree students, and the average age of matriculation to Emory University School of Medicine was 24 years (range 21-32 years).
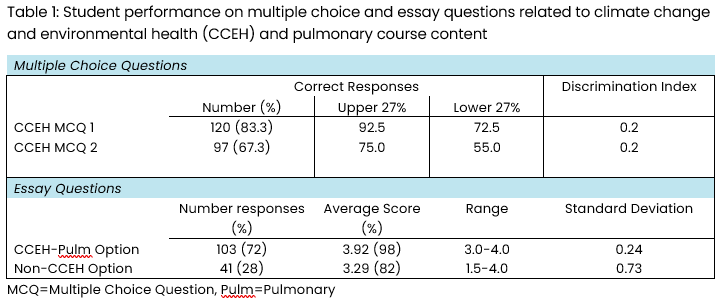
The overall mean and median score on the multiple-choice portion of the Pulmonary course final exam was 73%. For the CCEH multiple choice questions, more specifically, 83% and 67% of students correctly answered the first and second questions, respectively (Table 1). On both questions, student responses spanned all multiple-choice answer options. On the first question, 92.5% of the top-performing (upper 27%) of students answered the question correctly compared with 72.5% of the bottom-performing (lower 27%) of students, for a discrimination index of 0.2. For the second question, 75% of the top-performing students and 55% of the bottom-performing students answered the question correctly, for a discrimination index of 0.2. The overall mean score on the essay component of the Pulmonary course final exam, for which students responded to nine total questions, was 89%. Of the 144 students, 103 (72%) chose to answer the question prompt related to climate change, air pollution, and pulmonary health (referred to as the CCEH-Pulmonary essay), as opposed to its randomly paired prompt. The average score on the CCEH-Pulmonary essay was 3.92 out of a possible 4.0 points (range 3.0-4.0, 98%) compared with an average score of 3.29 (range 1.5-4.0, 82%) on the alternative essay option (Table 1).
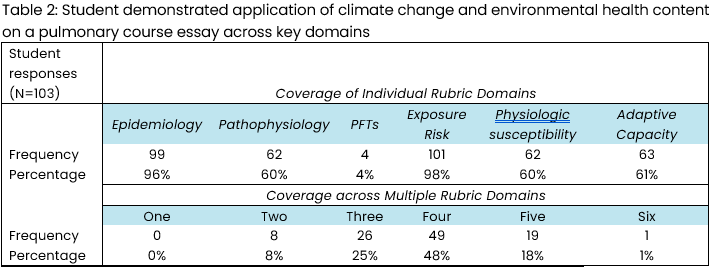
On the CCEH-Pulmonary essay, the 103 student essays overwhelmingly demonstrated applied understanding of the significance of exposure (98%, n=101) and epidemiology (96%, n=99) in the relationship between pollution and asthma. Fewer students demonstrated applied understanding of pathophysiology (60%, n=62), physiologic susceptibility (60%, n=62), and relevance of adaptive capacity (61%, n=63) in their responses. Only 4% (n=4) of students demonstrated applied understanding of the effects of air pollution exposure on pulmonary function tests (Table 2). Ninety-one percent of students (n=94) demonstrated application of their knowledge in three to five domains that were scored with the rubric, 8% (n=8) covered two domains in their responses, and a single student (<1%) covered all six domains.
This study illustrates the feasibility of seamlessly incorporating CCEH into all aspects of a pre-clinical course, including end-of-course assessments. Overall, students performed well on CCEH multiple choice questions and a short essay response during their final Pulmonology course exam. Specifically, student performance on the two CCEH-related multiple-choice questions was similar to the overall exam average, with neither falling more than two standard deviations from the mean. This indicates that the questions were well-matched in difficulty to the rest of the exam and effectively discriminated between higher- and lower-performing students. As a result, both multiple choice questions were retained for use in subsequent cohorts taking the exam.
Student essay responses suggest that the cohort completed the course with a strong grasp of the epidemiology of respiratory disease in relation to air pollution and the relationship between risk of exposure to air pollution and subsequent negative health implications. Students performed well on the CCEH essay question, even though the essay question required application—not just knowledge–of this relatively complex subject matter. Essay assessments are further up Miller’s Pyramid of Competency Evaluation than multiple choice questions and are commonly accepted to require greater cognitive engagement with the content and interpretation and application of key principles. Student performance on this question at 98% was higher than that for other essays. The student average performance on all essays was high at 89%, each essay question had an average score exceeding 80%, and three questions exceeded 90%.
The distribution of domains that students covered in their essay responses also suggests areas for improving both the curriculum and grading rubric. Most students did not discuss all three components of the environmental health vulnerability assessment framework, exposure risk, physiologic susceptibility, and adaptive capacity, in their responses. The exam rubric enabled students to achieve full points without demonstrating knowledge of this framework, a clear opportunity for improvement. In addition, the number of students who demonstrated understanding of the impact of air pollution on PFTs was strikingly lower than all other categories. In prior focus groups, students have asked for the CCEH curriculum to include more clinical application of CCEH content and pathophysiology (Liu et al., 2022). Meeting this need can be challenging, as preclinical students are still in the early stages of developing clinical reasoning skills and forming their professional identities as future physicians. A concrete example of relevant clinical tools, PFTs are covered in small groups in a workshop during the course, and all students participate in this workshop. Students’ seeming avoidance of discussing PFTs in their responses may reflect relatively less comfort with this aspect of the content covered in CCEH Thread in the Pulmonary Course. On the other hand, because the alternative essay prompt was on PFTs more specifically, the students who were most comfortable with PFTs may have chosen the alternate essay question. That said, the CCEH essay did not require students to discuss PFTs in their response, and the rubric enabled students to earn points in one domain without demonstrating application of knowledge across all domains. In the future, a more challenging question could require students to include consideration of PFTs, and a more challenging rubric could require students to earn points across a certain number of domains for full credit.
This study has several limitations and should be interpreted with caution. This analysis includes only one class year, leading to a small sample size and results that could be biased by temporality. While the results indicate that students understood key components of the relationship between fine-particle pollution and respiratory health, it is impossible to know whether students learned this in the formal curriculum or brought this knowledge from prior sources. The essay question introduces a component of subjectivity in the grading scheme that may have been exaggerated when senior student graders –who may not have received this content themselves—applied the rubric to junior students. Our independent evaluation of students’ demonstrated knowledge across key domains may have mitigated this limitation. Nevertheless, that authors only had access to the students’ final scores for the essay question (and not the detailed allocation of points) is a limitation. The Pulmonary course exam does include several other multiple-choice questions that emphasize environmental exposures and require students to apply an environmental health lens. However, this study only considers new questions directly related to novel CCEH content. Alongside these limitations, there are notable strengths to our approach, including evaluation of different question types and the involvement of students in every aspect of CCEH integration from creation of the content to teaching and evaluating the course.
Overall, the strength of student comprehension of CCEH as it relates to respiratory health indicates that the integration of climate change into the curriculum is advancing the CCEH knowledge of first-year students. Results will inform targeted revisions to course content, questions, and scoring rubrics, specifically to enhance understanding of PFTs in clinical care scenarios for patients exposed to air pollution. These findings demonstrate that climate and environmental health content can be effectively integrated into early medical education and assessed meaningfully, suggesting this strategy could be applied to similar –or similarly novel– content in other health professional training programs. Embedding climate-related clinical reasoning into the foundational training of nurses, physician assistants, public health professionals, social workers, and respiratory therapists, among others, can foster a shared interdisciplinary language while equipping future providers with the tools to recognize and respond to environmental health risks in both clinical and community settings.
Our results suggest that the integration of CCEH content into the pulmonology curriculum successfully builds upon students’ foundational climate and health knowledge and contextualizes CCEH content. The integration of CCEH assessment into an existing course is feasible and provides valuable information on student comprehension of CCEH knowledge as well as valuable information on strengths and opportunities for improvement of the curriculum. Integrating co-created assessment content within existing course assessments, mirroring the integrated and disseminated method for content delivery, offers a strategy for advancing climate education and incorporating other emerging topics in a wide range of health professions training.
The authors do not have any conflicts of interest to disclose. Dr. Philipsborn would like to acknowledge support from the Josiah Macy Jr Foundation that has helped to support this work.
Blood A, B. A., Speicher M, Farmakidis A. (2024, November 8-12). State of the Curriculum: Findings from the AAMC and AACOM Curriculum SCOPE Survey [Conference Presentation]. Learn, Serve, Lead: AAMC Annual Meeting, Atlanta, GA, United States.
D’Amato, G., Chong-Neto, H.J., Monge Ortega, O.P., Vitale, C., Ansotegui, I., Rosario, N., Haahtela, T., Galan, C., Pawankar, R., Murrieta-Aguttes, M., Cecchi, L., Bergmann, C., Ridolo, E., Ramon, G., Gonzalez Diaz, S., D’Amato, M., & Annesi-Maesano, I. (2020). The effects of climate change on respiratory allergy and asthma induced by pollen and mold allergens. Allergy, 75(9),2219-2228. https://doi.org/10.1111/all.14476
ExamSoft. (n.d.). ExamSoft: Assessment software for higher education. ExamSoft Worldwide, LLC. Retrieved from https://examsoft.com
Hampshire, K., Ndovu, A., Bhambhvani, H., & Iverson, N. (2021). Perspectives on climate change in medical school curricula—A survey of U.S. medical students. The Journal of Climate Change and Health, 4, 100033. https://doi.org/10.1016/j.joclim.2021.100033
Liu, I., Rabin, B., Manivannan, M., Laney, E., & Philipsborn, R. (2022). Evaluating strengths and opportunities for a co-created climate change curriculum: Medical student perspectives. Frontiers in Public Health, 10, 1021125. https://doi.org/10.3389/fpubh.2022.1021125
Mireku, N., Wang, Y., Ager, J., Reddy, R. C., & Baptist, A. P. (2009). Changes in weather and the effects on pediatric asthma exacerbations. Annals of Allergy, Asthma & Immunology: Official Publication of the American College of Allergy, Asthma, & Immunology, 103(3), 220–224. https://doi.org/10.1016/S1081-1206(10)60185-8
PHRC. (2024). Planetary Health Report Card 2023-2024 Summary Report: An International Health Student Initiative. Retrieved from https://phreportcard.org/wp-content/uploads/2024/04/MEDICINE-PHRC-2024-Summary-Report.pdf
Smirnova, N., Shaver, A. C., Mehta, A. J., Philipsborn, R., & Scovronick, N. (2023). Climate Change, Air Quality, and Pulmonary Health Disparities. Clinics in Chest Medicine, 44(3), 489–499. https://doi.org/10.1016/j.ccm.2023.03.005
Trilling, D. (2024, May 29). Bringing climate change into medical school. The Salata Institute. https://salatainstitute.harvard.edu/bringing-climate-change-into-medical-school/
Wellbery, C., Sheffield, P., Timmireddy, K., Sarfaty, M., Teherani, A., & Fallar, R. (2018). It’s Time for Medical Schools to Introduce Climate Change Into Their Curricula. Academic Medicine: Journal of the Association of American Medical Colleges, 93(12), 1774–1777. https://doi.org/10.1097/ACM.0000000000002368
Medical student, Emory University School of Medicine
Medical student, Emory University School of Medicine
Associate Professor, Division of General Pediatrics and Adolescent Medicine, Department of Pediatrics, Emory University School of Medicine, and Gangarosa Department of Environmental Health, Rollins School of Public Health, ORCID 0000-0002-2843-7509
Associate Professor, Division of Pulmonary, Allergy, Critical Care & Sleep Medicine, Department of Medicine, Emory University School of Medicine, ORCID 0000-0003-0287-8653, amehta4@emory.edu
Published: 7/21/25